Insurers are swimming in data. Most providers aren’t and that gap puts hospitals at a disadvantage in payer negotiations and ongoing performance management. While many organizations try to monitor contracts with homegrown dashboards, the underlying data quality often falls short.
Modern Revenue Cycle Analytics, especially prospective contract modeling embedded in Managed Care Software, closes that gap. It gives hospitals the leverage, clarity, and shared visibility to negotiate smarter and monitor outcomes continuously. These capabilities are the focus of PMMC’s whitepaper, Using Analytics to Drive Your Payer Contracts. Below are the three biggest advantages.
Data and Insights Driven by Accuracy Metrics
Many providers track the wrong indicators, making it hard to measure payer timeliness and accuracy or pinpoint root causes of variance. Prospective contract modeling emphasizes enhanced accuracy metrics (expected vs. actual allowables, line-level variance, payer-specific denial causality) so teams can:
- Spot anomalies earlier—before they snowball into revenue leakage
- Quantify true underpayments with defensible variance logic
- Prioritize high-yield opportunities for recovery and renegotiation
Real-Time Data Visualization
Immediate access to accurate, real-time business intelligence that affords the ability to easily drill down into the data for deeper, more detailed insights facilitates business solutions that address the root causes of problems before they can lead to more significant financial harm.
With robust revenue cycle analytics, leaders move from reactive reporting to proactive decisioning that protects cash flow.
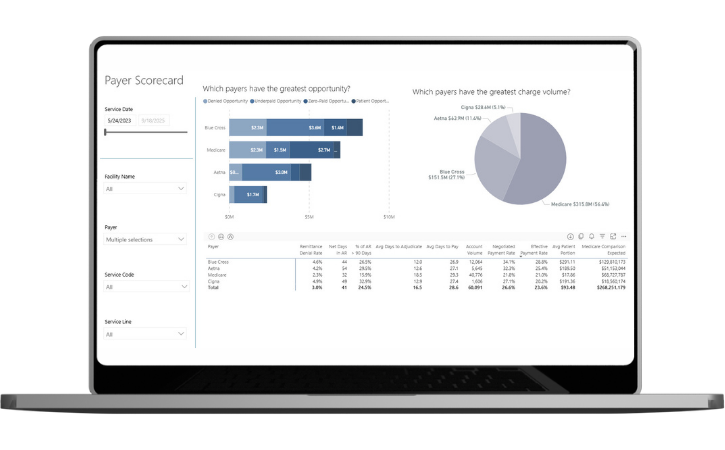
Payer scorecards help healthcare providers understand payer performance and identify opportunities for re-negotiating contract terms.
A Single Source of Truth That Brings Managed Care and Revenue Cycle Teams Together as Never Before
The use of prospective contract modeling analytics unites Managed Care and Revenue Cycle teams on one shared data backbone. This cohesion enhances productivity, reduces miscommunication, minimizes calculation errors and maximizes reimbursement opportunities.
PMMC recommends adopting this analytics-first approach not as a point solution, but as a core financial management strategy—so contracts are negotiated with precision and monitored continuously.



