Limited visibility into contract performance makes it difficult to identify and recover underpayments, leading to significant margin erosion.
Is Your Bottom Line Suffering from Managed Care Contract Complexities?

Are You Getting Paid Correctly?

Ready to Win Your Next Negotiation?
Fragmented, retrospective data limits benchmarking and scenario modeling, reducing negotiation leverage and leading to suboptimal contract outcomes.

Do Payers Have An Edge?
Outdated, delayed data keeps you reactive, limiting your ability to counter payer tactics and address performance issues in real time.

Unlock the True Value of Your Managed Care Contracts
We turn your data into a powerful negotiation tool. By bringing order and clarity to even the most complex data environments, we set you up for success with accurate models and actionable insights. This lets you benefit from more profitable contracts which means more revenue for your organization.
- Simplify complex data: Our easy-to-use system lets you seamlessly model infinite scenarios instantly, without getting bogged down in details.
- Strengthen payer negotiations: We arm you with accurate data and detailed analytics to help you navigate complex payer relationships and head to the negotiation table with confidence.
- Benchmark for success: We help you benchmark against your peers to ensure you are choosing the best terms for your organization and measure contract performance by comparing actual vs. expected outcomes.
- Provide ongoing support: You’ll receive comprehensive training and a dedicated Client Performance Manager to foster continuous learning and assist you as much or as little as you need.
Our goal is to ensure you are always armed with the best information, empowering you to make strategic decisions and secure the most favorable terms for your organization
Negotiate more profitable payer contracts
Our contract management system leverages accurate allowables and denial rates to empower your organization with precise financial insights. By utilizing these metrics, you can drive better contract models and better forecast reimbursement scenarios and identify potential revenue leakage. This ensures that you are not only optimizing contract performance but also proactively addressing problem areas to reduce denials and improve cash flow.
Comprehensive Data for Stronger Negotiations
We analyze your managed care contracts and claims data, combining it with payer benchmarks and historical trends. This gives you a complete picture of your performance and helps you secure the best possible contract terms for your organization.
Experienced Professionals Who Understand Your Challenges
With extensive knowledge of revenue cycles and managed care challenges, our team brings years of expertise to the table. We go beyond basic analysis, offering strategic solutions that simplify contract management and create long-term value.
A Dedicated Partner
We act as an integrated part of your team, providing proactive and compliant solutions to enhance your managed care strategy. Our support equips you with the tools and confidence needed to maximize revenue, improve efficiency, and secure better financial outcomes.
Innovative Technology for Effective Modeling
PMMC’s Xact EngineSM and AI tools are specifically designed to handle the complexities of healthcare finance. We simplify managed care contract modeling by assessing contract terms from various angles and using comprehensive datasets. This approach provides you with the actionable insights needed to negotiate more favorable terms and enhance your financial results.
Streamlined Modeling for Results
Our methodologies accelerate the contract negotiation process, identifying opportunities for improvement and revenue uplift with unmatched speed. PMMC not only produces in-depth financial models but also delivers clear, actionable strategies that help maximize reimbursement and strengthen your negotiating position.
Actionable Data for Strategic Decision-Making
We cut through the noise of managed care data, delivering the clarity you need to act decisively. Our sophisticated analytics simplify complex information with instant calculations and intelligent workflows, helping you identify critical trends, explore unlimited “what-if” scenarios, and make financial decisions that drive sustainable growth.
A Flexible Approach, Tailored to You
Our services adapt to your organization’s unique needs. Whether you require comprehensive support or a more hands-off approach, our experts integrate with your team to deliver results that align with your strategic goals.
Accuracy Starts with Smarter Intelligence
PMMC’s accuracy advantage is rooted in advanced technology and healthcare-specific expertise. Here’s how it connects with managed care roles:
 The Xact Engine SM
The Xact Engine SM
- Designed specifically for healthcare finance, PMMC’s Xact EngineSM ensures precision by analyzing financial performance through multiple data lenses.
- Managed care roles benefit from this comprehensive approach, enabling more reliable payer reimbursement calculations.
 More Data. Better Insight.
More Data. Better Insight.
- By leveraging over 20+ data types, including external and market-based sources, PMMC creates a clear and detailed financial picture.
- Managed care professionals gain actionable insights for negotiation and decision-making with unprecedented accuracy.
 Term-by-Term Contract Integration
Term-by-Term Contract Integration
- PMMC’s contract specialists meticulously input and validate contracts to ensure 99.8% accuracy in processing.
- This precision empowers managed care teams to confidently address payer mixes and ensure financial compliance.
 Proprietary Processes and Industry-Leading Speed
Proprietary Processes and Industry-Leading Speed
- PMMC’s unique methodologies and rapid calculation capabilities accelerate insights for maximum impact.
- Managed care teams benefit from faster, more effective financial analytics that support real-time strategy adjustments.
By combining smarter intelligence, comprehensive data integration, and proprietary processes, PMMC ensures unparalleled accuracy in healthcare financial management.

Triple E Service: Extreme Engagement & Excellence
At PMMC, we understand that every organization is unique. That’s why our Triple E Service model adapts to your specific needs, team dynamics, and operational pace, delivering the precise level of support you require. We purposefully recruit professionals with extensive experience in hospital revenue cycle operations and healthcare data analytics.

Contract Models
- PMMC’s contract models include advanced analytics and benchmarking tools specifically designed for managed care leaders to efficiently evaluate payer contracts and identify potential improvement areas.
- Their user-friendly dashboards provide clear insights into payment schedules and performance metrics, simplifying the decision-making process.
- These models drive smarter negotiations and enhance revenue optimization by highlighting underperforming contracts.
- They also promote operational efficiency by reducing administrative burdens and improving financial predictability.

DocumentsAISM
DocumentsAISM streamlines your managed care operations by automating document workflows, providing actionable insights, and optimizing contract terms. Its intuitive platform helps improve efficiency, minimize errors, and save time so your team can prioritize what truly matters: securing better payer contracts. By converting existing agreements into a structured database, it transforms contract modeling efforts
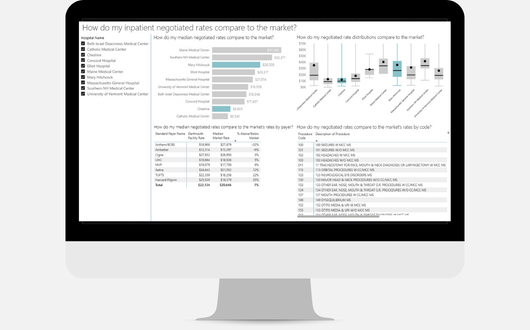
Negotiated Rate Analytics
PMMC’s Negotiated Rate Analytics empowers managed care teams with actionable insights into payer reimbursement rates across your specific market. By leveraging our comprehensive data, teams can pinpoint high-value opportunities, benchmark internal performance against competitors, and identify critical discrepancies in contract terms. This specialized intelligence enables more informed decision-making, fostering strategic negotiations that align with your organizational goals and secure a sustainable competitive advantage.

Revenue Cycle Analytics
- PMMC’s Analytics+ tools deliver real-time insights into key managed care metrics, helping organizations track trends and make informed decisions.
- The platform integrates effortlessly with existing systems, providing customizable dashboards and detailed reporting. For managed care leaders, this means enhanced visibility into contract rates and improved modeling, allowing for greater control over payer negotiations and financial outcomes.
- With PMMC’s advanced solutions, leaders can streamline processes, improve payer negotiations, and maximize revenue opportunities across their networks.
Report Examples:
- Executive Contract Rates Dashboard, Comparison Simulations
- Contract Rates, Service Lines, Patient Liability & Underpayments, Outliers & Add Ons
- Contract Rate Optimization Comparisons
- Lesser-of Charges Impact Reports
- Denial and Underpayment Reports to support negotiations
- Reimbursement Methodology Distribution

Talk With An Expert
Have questions about solutions built for the unique challenges of your managed care team? Let’s connect and discuss your specific challenges and needs.
Superior Managed Care Software & Insights
Transform Managed Care Operations with Software and Modeling
To thrive and deliver optimal results, you require advanced tools and strategies that enable you to manage contracts, optimize reimbursements, and negotiate better rates efficiently. Managed care software and managed care contract modeling have emerged as critical components for achieving these objectives, allowing organizations to streamline operations and improve financial outcomes.
The Importance of Managed Care Contract Modeling
Managed care contract modeling is at the heart of efficient healthcare operations. This process empowers managed care companies to evaluate the financial implications of payer contracts, negotiate better terms, and adapt to changing reimbursement methodologies. By using accurate data and insights, healthcare leaders can simulate multiple contract scenarios, ensuring they identify the most favorable terms while managing financial risks.
Key tools like a Contract Rates Dashboard or Comparison Simulations provide valuable insights into contract performance. These tools allow organizations to oversee rates, compare with market benchmarks, and identify potential areas of improvement. For instance, understanding the impact of contract rates on service lines, patient liability, and underpayments can significantly improve negotiations with payers. Additionally, Lesser-of Charges Impact Reports and Outliers and Add Ons Analysis offer deeper clarity into financial metrics that directly affect reimbursement strategies.
How Managed Care Software Maximizes Efficiency
Managed care software acts as a foundation for innovation and efficiency within healthcare organizations. This technology centralizes data, automates repetitive tasks, and provides actionable analytics to support decision-making. With proper implementation, managed care companies can reduce administrative burden and focus on core functions like improving patient care and refining operational strategies.
One of the key capabilities of managed care software includes access to advanced analytics and reporting, specifically reports like a Denial and Underpayment Report. These reports highlight areas where payers are not meeting their obligations, flagging denials that need to be addressed. By reviewing payment trends and denial data, healthcare organizations can better prepare for contract renegotiations, addressing payment inconsistencies upfront.
Further insights are provided by Reimbursement Methodology Distribution reports, which map out how payments are structured across different payers. This granular analysis is crucial for recognizing when fee schedules, bundled payments, or performance-based reimbursements are beneficial to the organization.
Leveraging Data for Optimal Decision-Making
The success of managed care teams is heavily reliant on their ability to interpret data effectively. Managed care software serves as a hub for storing and analyzing information, helping leaders track financial trends and operational outcomes over time. For example, insights from Contract Rate Optimization Comparisons make it easier to pinpoint the contracts yielding the highest returns and identify whether adjustments are necessary.
These features also benefit contract modeling. Healthcare organizations can use the data and simulations generated by managed care software to test various “what-if” scenarios. Such simulations include examining changes in payer rates, the introduction of new reimbursement models, or the impact of volume shifts on contract revenue. These proactive initiatives prevent costly surprises, preparing organizations to act strategically.
Preparing Managed Care Companies for the Future
The healthcare industry is under constant pressure to deliver quality care at a lower cost, amid regulatory changes and increasing patient demands. Managed care companies need to rely on both managed care contract modeling and cutting-edge software to remain competitive. These tools enable organizations to achieve financial stability by highlighting inefficiencies, missing revenue opportunities, and suboptimal payer agreements.
For healthcare organizations to succeed in today’s market, investing in managed care software and contract modeling tools is no longer optional—it’s essential. These innovations allow healthcare leaders to not only manage their contracts more effectively but also prepare for an uncertain and demanding future. Managed care teams that adopt this transformational technology will be better equipped to meet growing expectations while maintaining financial performance.

